Few dental procedures carry as much undeserved fear as root canals. Ask almost anyone, and they’ll tell you it’s the one thing they dread most, yet the majority of patients who actually go through with it say it was nothing as they expected. Modern root canal therapy is performed under local anesthesia, and for most people, the procedure itself is no more uncomfortable than getting a filling. The pain people associate with root canals is almost always the pain they were already feeling — from the infected tooth, not from the treatment.
Still, it’s completely reasonable to want to know what you’re walking into. This guide covers what root canal treatment actually involves, what the discomfort really looks like (before, during, and after), and what you can do to have the smoothest possible experience.
What’s Happening Inside the Tooth?
To make sense of the procedure, it helps to know what’s going on inside a tooth that needs a root canal. Each tooth has an inner chamber called the pulp, which contains nerves, blood vessels, and connective tissue. This pulp is essential during tooth development, but once a tooth is fully mature, it can function without it.
When bacteria reach the pulp through deep decay, a cracked tooth, or repeated dental procedures on the same tooth, infection sets in. The pulp becomes inflamed, and that inflammation creates pressure inside the tooth that has nowhere to go. That’s the source of the throbbing, sometimes severe pain that drives people to the dentist in the first place.
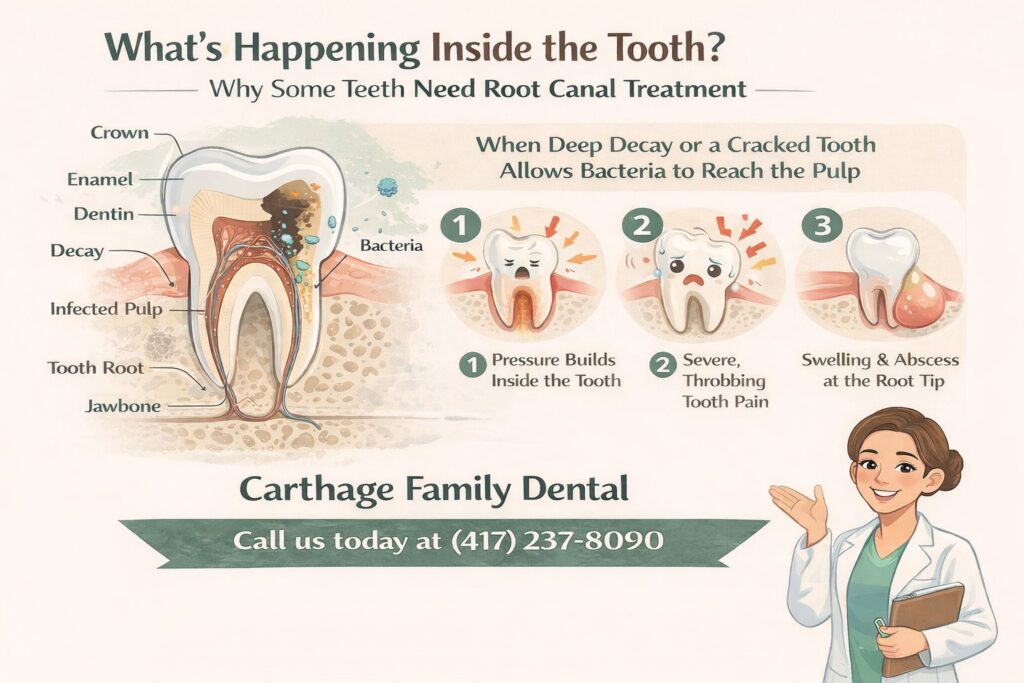
Root canal therapy in Carthage removes the infected pulp, cleans and shapes the canals inside the tooth roots, and seals everything off to prevent reinfection. The nerve is gone after treatment, which means the tooth no longer sends pain signals. That’s a relief, not a loss.
Pain Before Treatment: Why the Tooth Hurts So Much
The discomfort most people attribute to root canal treatment is actually the infection itself talking. Pulpitis – inflammation of the pulp can cause an intense, persistent toothache that worsens with heat, pressure, or lying down. Some patients also develop a dental abscess, which is a pocket of pus at the root tip that can cause swelling in the jaw or face.
By the time a root canal is recommended, the tooth is often already causing significant pain. The procedure doesn’t create that pain – it ends it. Most patients report noticeable relief within a day or two of treatment, once the infected tissue is removed and the inflammation begins to resolve.
Delaying treatment tends to make things worse, not better. Dental infections don’t resolve on their own. They spread, and in rare cases, an untreated abscess can become a serious medical concern. If you’re in pain, getting seen promptly is genuinely the most important thing you can do.
What the Procedure Feels Like
Here’s the part most people want to know. A root canal appointment typically begins the same way as any other dental procedure: with a local anesthetic injection to numb the tooth and surrounding tissue. Your dentist or endodontist will wait until the area is fully numb before proceeding, and they can give additional anesthetic if needed at any point.
Once you’re numb, the procedure itself involves:
- Creating a small opening in the top of the tooth to access the pulp chamber
- Using fine instruments called files to remove the infected pulp and shape the canals
- Irrigating the canals thoroughly with an antimicrobial solution to eliminate remaining bacteria
- Filling and sealing the canals with a rubber-like material called gutta-percha, then placing a temporary or permanent filling
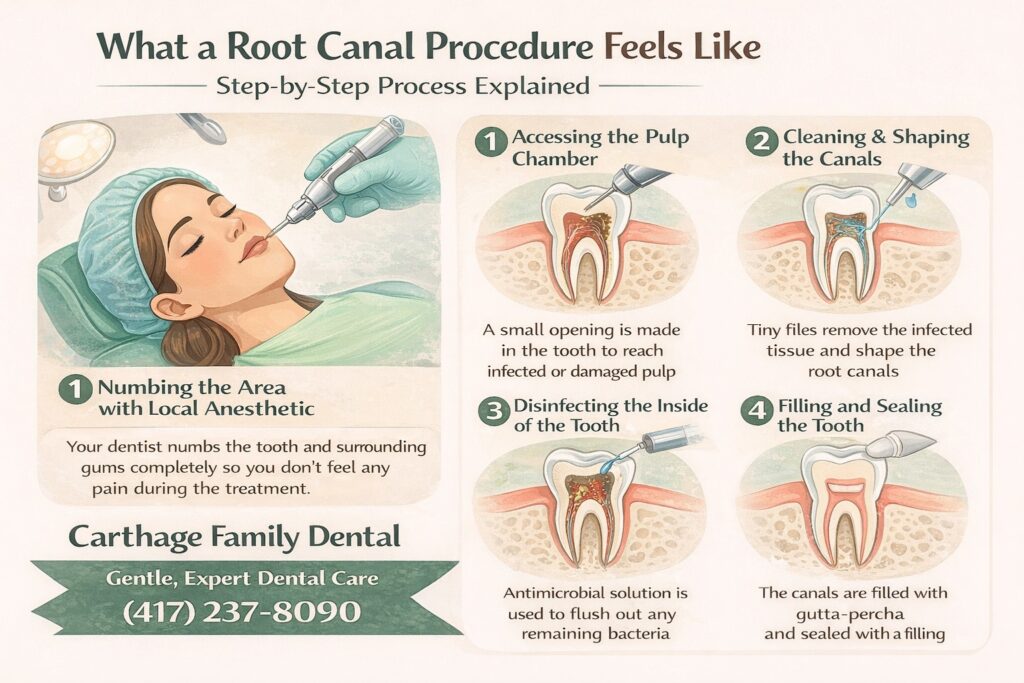
Most patients feel pressure during the procedure, but not sharp pain. Some experience brief sensitivity if the anesthetic wears off unevenly. If that happens, you should tell your dentist immediately so they can re-numb the area. You don’t have to white-knuckle through anything.
What to Expect After the Appointment
Once the anesthetic wears off, some soreness in the treated area is normal for a few days. The tooth itself may be tender to biting pressure, and the gum tissue around it can feel sensitive. This is your body’s normal inflammatory response to the procedure — not a sign that something went wrong.
Over-the-counter pain relievers like ibuprofen or acetaminophen manage post-treatment discomfort effectively for the majority of patients. Your provider may also prescribe a short course of antibiotics if the infection is significant. Most people return to their normal routine the day after treatment.
The final step (a dental crown placed over the treated tooth) is usually scheduled as a separate appointment. A crown restores the tooth’s full function and protects it from fracture, which is particularly important for back teeth that absorb the most chewing pressure.
Signs You Might Need a Root Canal
Not every toothache means a root canal is on the way, but certain symptoms suggest the pulp may be involved. Worth mentioning to your dentist promptly:
- Persistent, deep toothache that doesn’t resolve or gets worse over time
- Prolonged sensitivity to heat or cold that lingers after the stimulus is removed
- Pain when biting or chewing on a specific tooth
- Darkening of a tooth compared to the ones beside it
- Swelling, tenderness, or a pimple-like bump on the gum near a tooth
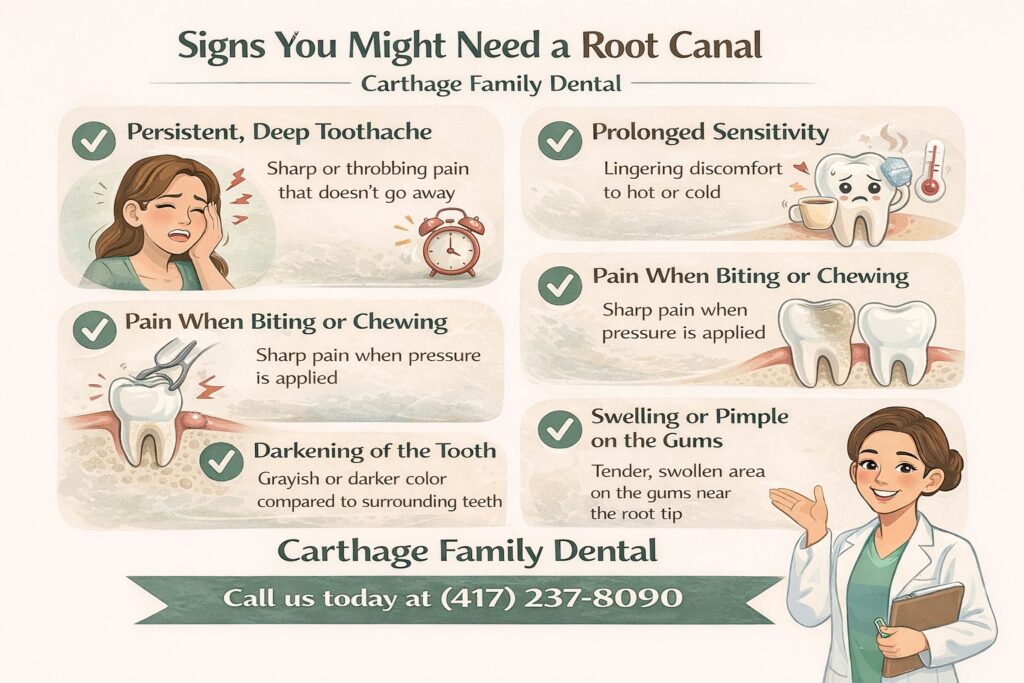
None of these is an indubitable diagnosis on its own, but they’re worth taking seriously. An X-ray and clinical exam will tell your dentist what’s happening at the root level.
Don’t Let Fear Delay the Care You Need
Root canal treatment has changed dramatically over the past two decades. The techniques are more precise, the anesthetics are more effective, and the recovery is faster than most people expect. What hasn’t changed is that a tooth infection won’t get better on its own — and the sooner it’s addressed, the simpler the treatment tends to be.
Carthage Family Dental offers root canal therapy in Carthage in a calm, patient-focused environment where your comfort is taken seriously from the moment you walk in.
→ Call (417) 526-4170 or book online today to schedule your appointment.
FAQs About Root Canal Treatment in Carthage
Most root canals are completed in one or two appointments. Straightforward cases on front teeth often finish in a single visit. Molars with multiple canals or severe infections may require a second appointment to ensure everything is fully cleaned before the final seal is placed. A separate crown appointment typically follows once the tooth has settled.
Yes, though it’s uncommon when the procedure is done properly, and the tooth is protected with a crown. Reinfection can occur if bacteria re-enter through a cracked restoration, a new cavity, or an incomplete seal. A procedure called an apicoectomy — a minor surgical option — can address persistent infection at the root tip if retreatment alone isn’t sufficient.
Saving a natural tooth is almost always the preferred outcome when it’s clinically viable. A root canal preserves your tooth and its root, which maintains the jawbone beneath it and keeps neighboring teeth in position. Extraction creates a gap that can shift surrounding teeth and may require a bridge or implant to restore function — both of which involve additional procedures and time.
The infection will not resolve without treatment. Over time, it can spread to surrounding teeth, the jawbone, or nearby tissue. In severe cases, a dental abscess can become a systemic health issue. The tooth will likely need extraction eventually, except that by that point, there may be additional bone loss or damage to address.
Absolutely, and good dental providers plan for it. If you have significant anxiety around dental procedures, let your dentist know ahead of the appointment. Options like nitrous oxide (laughing gas) or oral sedation can be used to help you stay calm and comfortable throughout. There’s no reason to avoid necessary care because of anxiety – there are practical tools to address it.
